Allergic Conjunctivitis
What is allergic conjunctivitis?
Allergic conjunctivitis is a common eye problem that affects roughly about 1 in 5 children. It happens when the thin layer covering the white part of the eye (called the conjunctiva) reacts to things that cause allergies. These things are called allergens. Common allergens include dust, pollen, pet dander, and sometimes medicines.
When allergens touch the eyes, they can make the eyes itchy, red, watery, swollen, or irritated. The symptoms may look like an eye infection, but allergic conjunctivitis is not an infection and is not contagious.
WHAT CAUSES ALLERGIC CONJUNCTIVITIS?
Allergic conjunctivitis starts when the eye touches something a person is allergic to. Pollen from trees, grass, weeds, or flowers often causes allergies in the spring, summer, or fall. Some people have allergies all year from things inside the home, like dust, mold, or pet hair. Children with other health problems, such as asthma or eczema, may be more likely to get allergic eye conditions.
WHAT ARE SOME COMMON SYMPTOMS OF ALLERGIC CONJUNCTIVITIS?
The main symptom is itchy eyes. If the eyes are not itchy, it is usually not an allergy. Other symptoms include:
- Burning, stinging, or tearing
- Red or pink eyes
- Swelling around the eyes or eyelids
- Tiny bumps on the surface of the eye
- Eyelids that are red, thick, or itchy
Children may rub their eyes often, blink a lot, or squeeze their eyes shut to help with the itching. Symptoms are usually worse in spring and summer but can happen year-round. Bright light may bother the eyes when allergies are severe.

Fig. 1: A red or pink eye with itching is a typical sign of allergic conjunctivitis.
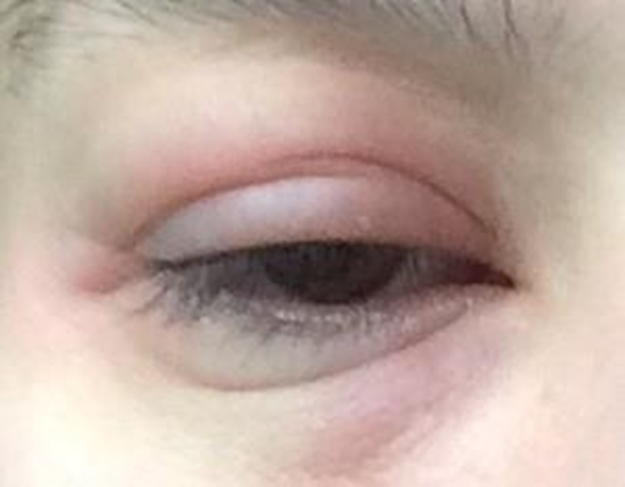
Figure 2. Swelling and redness of the eyelids can also occur with allergic conjunctivitis.
IS ALLERGY TESTING NECESSARY?
Doctors usually diagnose allergic conjunctivitis by asking questions and looking at the eyes. Allergy tests are rarely needed because the triggers (pollen, dust, pets) are common. Treatment is usually the same no matter what allergen is causing the problem.
HOW DO YOU TREAT ALLERGIC CONJUNCTIVITIS?
The first step is avoiding allergens:
- Stay indoors when pollen counts are high.
- Wear glasses or goggles outside.
- Wash pillowcases and bedding often.
- Vacuum carpets in the bedroom.
- Wash the face and hair to remove allergens.
Artificial tears (eye drops) can rinse allergens out of the eyes and help calm inflammation. Keeping drops cold in the refrigerator may give extra relief. It is also important to avoid rubbing the eyes, as this can make allergic conjunctivitis worse.
WHAT MEDICATION(S) ARE AVAILABLE TO TREAT ALLERGIC CONJUNCTIVITIS?
Eye drops for allergies are sold both with and without a prescription. Some need to be used every day for weeks, while others work when used only as needed. Eye drops often work better than pills or liquid medicines because they act directly on the eyes and don’t cause drowsiness. Pills or liquids may help if swelling is severe or if other allergy symptoms, like runny nose, are also present. Please speak with your ophthalmologist if you have questions about allergy medications.
WHAT IF ALLERGY DROPS ARE NOT HELPING??
Sometimes one type of eye drop may not work, but another type might. If symptoms do not improve, the doctor may suggest adding pills or liquid allergy medicine. These may also be helpful for children who have trouble using drops.
ARE STEROID EYE DROPS SAFE FOR CHILDREN?
Steroid eye drops are sometimes used for severe forms of allergies. These drops must be monitored closely by an ophthalmologist because using them too much or for too long can cause serious problems with the eye such as glaucoma, cataracts and eye infections (keratitis). Steroid drops should only be prescribed and monitored by an ophthalmologist. Talk with your child’s ophthalmologist if you have questions about steroid drops.
PROGNOSIS
Most children with allergic conjunctivitis do not lose vision. With proper care, symptoms usually improve. Problems can happen if eye rubbing is too hard, if infections develop, or if steroid drops are not used safely.
WHAT IS VERNAL CONJUNCTIVITIS?
Vernal conjunctivitis is a more serious type of allergic conjunctivitis. It is more common in boys and in places with hot, dry weather. Often, patients with vernal conjunctivitis also have asthma or eczema.
This condition causes strong symptoms that are often worse in spring (vernal means spring in Latin) and summer. Children may need both steroid and allergy eye drops. Special immune based medicines, such as cyclosporine eye drops, may also be needed. Big bumps called papillae on the inside of the eyelid are a common sign (Figure 2). Most children outgrow vernal conjunctivitis in their teenage years.

Fig. 2: Large bumps (papillae) inside the upper eyelid in vernal conjunctivitis.
SUMMARY FOR PATIENTS AND CAREGIVERS
Allergic conjunctivitis is an eye condition that causes itching, redness, tearing, and swelling when the eyes react to pollen, dust, or pet dander. It is not an infection and cannot spread to others. Avoiding allergens, rinsing the eyes with artificial tears, and using allergy eye drops are the main forms of treatment for this condition. Sometimes allergy medications given by mouth may be also needed. With proper care, most children’s symptoms improve and vision is not affected. Severe types of allergic eye disease also exist and may need stronger treatment options. Allergic eye disease usually improves as children get older.
For more information on allergic conjunctivitis and vernal conjunctivitis see:
https://eyewiki.org/Allergic_Conjunctivitis
https://eyewiki.aao.org/Vernal_Keratoconjunctivitis
Updated 08/2025
#Conditions